A little bit of history
1914
Carbon dioxide has been in use firstly as an imaging agent in radiology since 1914 to evaluate the retroperitoneum, to image kidneys, tumors and for venous system inspections.
70s
In the early 70s, Dr. Hawkins started using and studying the carbon dioxide as a contrast agent also for peripheral vascular imaging and intervention, after an accidental air injection.
80s
An improvement on the reliability of CO2 imaging came up in the 80s with the advent of the Digital Subtraction Angiography (DSA): image is calculated starting from an initial mask.
Today
Today CO2 is used as an alternative contrast agent to the standard ones. Technological improvements of dedicated injectors and imaging SW allow its daily use.
Carbon Dioxide as Contrast Agent
Being naturally present in the human body, CO2 is the only 100% biocompatible contrast agent: it has any adverse reactions, like allergies, nephrotoxicity and hepatotoxicity, as the human body knows how to manage this gas once it is injected.
Carbon dioxide is a negative contrast agent: it has a low radiopacity. Contrast is caused by the different X-ray absorption coefficients between the tissue and the contrast agent. In the vascular CO2 imaging, vessels look brighter rather than the surrounding tissues, as CO2 does not absorb X-ray radiations.
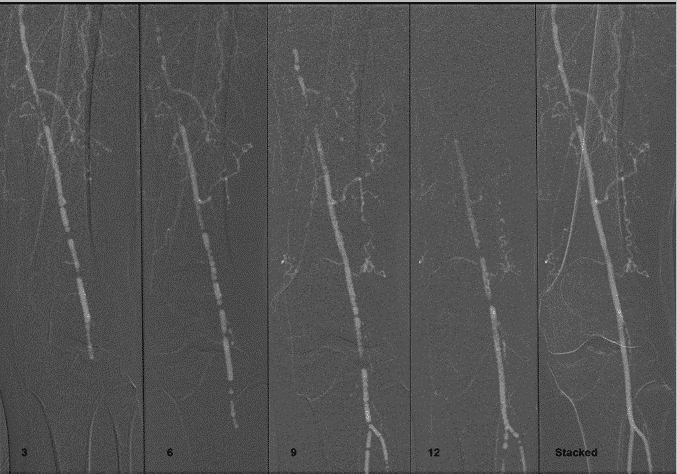
CO2 does not mix with blood . As it is a gas, CO2 forms a train of bubbles once injected, which displaces blood, causing a transient ischemia in relation to the bloodstream. Using the DSA " stacking " software, frames sum composes the final image.
CO2 is highly soluble : it dissolves quickly after a few seconds. CO2 is more than 20 times more soluble than Oxygen, meaning the possibility of injecting high quantities in the body. Multiple injections are possible, considering an adequate time interval to allow the gas to be expelled from the body.
High compressibility: more the pressure, more the density, less the gas volume. CO2 injection by catheter can lead to a sudden increase in gas volume ("jet effect") and to a wall stress. With a catheter flush with CO2, compression is reduced and steady flow rate is ensured during injection.
It is 400 times less viscous than iodine: CO2 can be injected through very little lumens, like microcatheters or residual lumen of devices. CO2 can pass through small vessels , visualizing tight stenoses, collaterals, small bleedings and endoleaks in AAA procedures.
Once dissolved in plasma, the gas is transported to the lungs and removed in a single pass: CO2 is simply breathed out. This let the possibility of multiple injections without complications. There are no implications for the kidneys, liver or other tissues.
Being lighter than blood, CO2 floats above the bloodstream. The main advantage is the simplicity of filling the more superficial body vessels.